Study of infant mortalities from heart defects finds while death rates decreased, white infants more likely to survive than Black infants
ORLANDO, Fla.— Some babies are born with abnormalities involving the structure of the heart, known as congenital heart disease (CHD). While many studies have shown that more babies with congenital heart disease are surviving past their first birthday as deaths from CHD have significantly decreased in the United States, a research abstract found that race impacts these survival rates.
Black infants with congenital heart disease are 40% more likely to die in the first year of life than white infants with congenital heart disease, according to research presented during the American Academy of Pediatrics 2024 National Conference & Exhibition at the Orange County Convention Center from Sept. 27-Oct. 1.
The research, “Trend in Racial Differences in Mortality Attributed to Congenital Heart Diseases in Infants in the United States from 2005 to 2019," found that improvements in death rates for children with heart abnormalities were due to reduced death rates for white babies with congenital heart disease.
“The death rate in white infants decreased significantly but the rate in Black infants did not. Overall, we also found that Black infants died from these abnormal heart structures at a rate that was 1.4 times that of white infants,” said lead author Kwadwo Danso, MBChB.
Researchers examined data from the Centers for Disease Control and Prevention on 60,243,988 live births, which included 19,004 congenital heart disease-related infant deaths, to investigate if death rates varied based on race for children born with CHD. They found that the overall congenital heart disease infant mortality rate declined from 36.1 to 27.0 per 100,000 live births, down 25.2%. However, throughout the study, Black infants with congenital heart disease died at higher rates.
“Our findings may have implications for patient care and public health policy by serving as a foundation for additional studies to determine the drivers behind these disparities,” Dr. Danso said. “More research is needed on this disparity to understand why Black infants with congenital heart disease are more likely to die.”
Study author Kwadwo Danso, MBChB, is scheduled to present the research, which is below, during the Section on Cardiology and Cardiac Surgery program at the AAP’s National Conference and Exhibition.
Media contact: Dr. Danso may be reached at (815) 603-7421 or [email protected]
Please note: only the abstract is being presented at the meeting. In some cases, the researcher may have more data available to share with media, or may be preparing a longer article for submission to a journal.
# # #
The American Academy of Pediatrics is an organization of 67,000 primary care pediatricians, pediatric medical subspecialists and pediatric surgical specialists dedicated to the health, safety and well-being of infants, children, adolescents and young adults. For more information, visit www.aap.org. Reporters can access the meeting program and other relevant meeting information through the AAP meeting website at http://www.aapexperience.org/
Abstract
Program Name: 2024 AAP National Conference-Abstracts
Submission Type: Section on Cardiology & Cardiac Surgery
Abstract Title: Trend in racial differences in mortality attributed to Congenital Heart Diseases in infants in the United States from 2005 to 2019
Kwadwo Danso
Peoria, IL, United States
Deaths from congenital heart disease (CHD) in children have been decreasing. We examined the differences in CHD mortality trends between Non-Hispanic Black (NHB) and Non-Hispanic White (NHW) infants in the United States from 2005 to 2019. We hypothesized that a disparity in mortality rates exists between NHB and NHW infants.
We performed a retrospective cross-sectional analysis of publicly available data from the Centers for Disease Control and Prevention’s Wide-ranging Online Data for Epidemiologic Research. The data was obtained from the linked birth/infant deaths from 2005 to 2019. We evaluated all infant deaths up to 1 year of age with the cause of death listed as CHD (International classification of diseases, 10th revision (ICD-10) codes Q20-Q26 (except atrial septal defect, Q21.1 and patent ductus arteriosus, Q25. CHD infant mortality rate (IMR) was calculated per 100,000 live births. Race was ascertained based on death certificate reporting. Joinpoint regression was used to examine CHD-IMR by year, including stratification by NHB vs NHW. The difference between NHB and NHW CHD-IMR was ascertained via the Mann-Whitney U test. P< 0.05 was considered statistically significant.
Out of 60,243,988 live births, there were 19,004 CHD-related infant deaths. The characteristics of the study population are displayed in Table 1. The overall CHD-IMR declined from 36.1 to 27.0 per 100,000 live births (25.2%) with an average annual percentage change (AAPC) of -2.1 [95% confidence interval (CI)-2.6, -1.572] (Figure 1). The CHD-IMR was significantly higher in NHB than in NHW (40 vs 29.3; P< 0.0001) and this difference remained when the CHD mortality rate was stratified by the neonatal and post-neonatal period. The CHD-IMR decreased significantly in NHW [AAPC: -2%; 95% CI: -2.5, -1.5%], however, it was not significant in NHB [AAPC of -1.4%, 95% CI, -3.0, 0.3%]. The NHB-to-NHW CHD-IMR ratio, a measure of CHD-IMR disparity averaged 1.4 and there was no significant change during the study period [AAPC: 0.8%; 95% CI: -0.2, 1.8%] (Figure 2).
The CHD-IMR declined significantly for NHW, but not in NHB in the US from 2005 to 2019. The CHD-IMR was significantly higher in NHB than in NHW. There was no significant change in the NHB-to-NHW CHD-IMR ratio, signifying no change in the disparity that exists between NHB and NHW IMR. These findings may have implications for patient care and public health policymaking. They lay the groundwork for additional studies to determine and understand the drivers behind these findings such as in prenatal diagnosis.
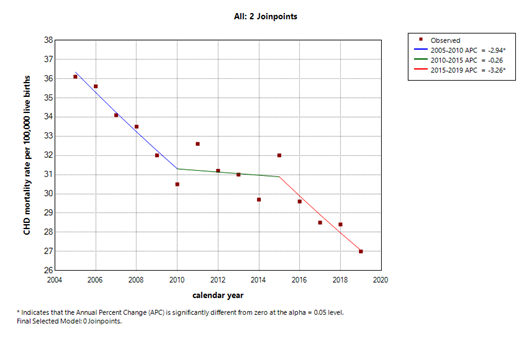
Figure 1 shows the overall CHD-IMR decline over the study period
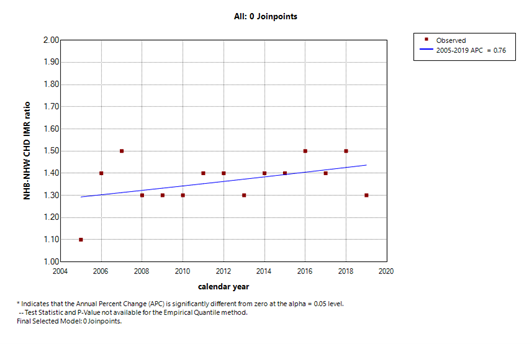
Figure 2 shows the NHB-NHW CHD IMR ratio over the time